If you are in distress, you can call or text 988 at any time. If it is an emergency, call 9-1-1 or go to your local emergency department.
- Fact sheets, Research
The crossroads of opioid use and suicide: let’s meet people where they need us
This resources was published in 2020. The data may be out of date. Opioid use and suicide share many of the same risk factors – and the same protective factors. Addressing them can help prevent suicides and reduce the harms of opioid use. When we talk about suicide and opioid use, we must consider the circumstances people live in and how to improve outcomes by addressing trauma, adverse childhood experiences, socio-economic factors, chronic pain, and discrimination. We also need to break down the barriers between mental health and addiction care, which often prevent people from receiving treatment from one if they’re getting help from the other.Facts
What can we do?
Shared Risk and Protective Factors
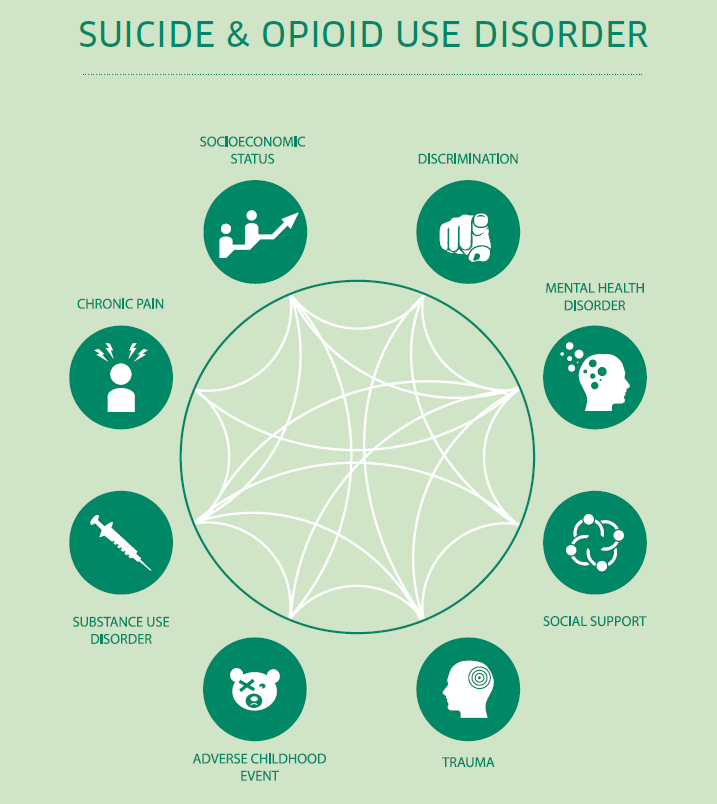
- Fact sheets, Research
The crossroads of opioid use and suicide: let’s meet people where they need us
The crossroads of opioid use and suicide: let’s meet people where they need us
- Health-care, Mental Health and Substance Use, Opioids, Suicide Prevention
This resources was published in 2020. The data may be out of date. Opioid use and suicide share many of the same risk factors – and the same protective factors. Addressing them can help prevent suicides and reduce the harms of opioid use. When we talk about suicide and opioid use, we must consider the circumstances people live in and how to improve outcomes by addressing trauma, adverse childhood experiences, socio-economic factors, chronic pain, and discrimination. We also need to break down the barriers between mental health and addiction care, which often prevent people from receiving treatment from one if they’re getting help from the other.
Facts
What can we do?
Shared Risk and Protective Factors

SHARE THIS PAGE
RELATED

Review our Assessment Framework for Mental Health Apps — a national framework containing key standards for safe, quality, and effective mental health apps in Canada.

To help expand the use of e-mental health services, we developed four online learning modules based on our Toolkit for E-Mental Health Implementation, in collaboration with the Centre for Addiction and Mental Health (CAMH).
Stepped Care 2.0© (SC2.0) is a transformative model for organizing and delivering evidence-informed mental health and substance use services.

